Lorem ipsum dolor sit amet, consectetur adipiscing elit, sed do eiusmod tempor incididunt ut labore et dolore magna aliqua. Ut enim ad minim veniam


A Multi-Disciplinary Approach to Managing Hypermobility Conditions in Children
Children with hypermobility conditions such as Paediatric Generalised Joint Hypermobility (pGJH), Paediatric Hypermobility Spectrum Disorder (pHSD), and Loeys-Dietz Syndrome (LDS), amongst others, often experience a range of challenges, including pain, fatigue, poor coordination, digestive issues, and emotional distress. Given the complexity of these conditions, a multi-disciplinary approach is essential to provide comprehensive, individualised care. Collaboration between healthcare professionals ensures that all aspects of the child’s well-being—physical, functional, social and psychological—are addressed effectively.
That's what we're all about as OTs, right? We see the WHOLE PERSON in their contexts and environments, and we aim to support them in engaging in meaningful occupations.
So let's break down the roles of the most common disciplines working with kids with hypermobility (this is not exhaustive):
Occupational Therapy (OT)
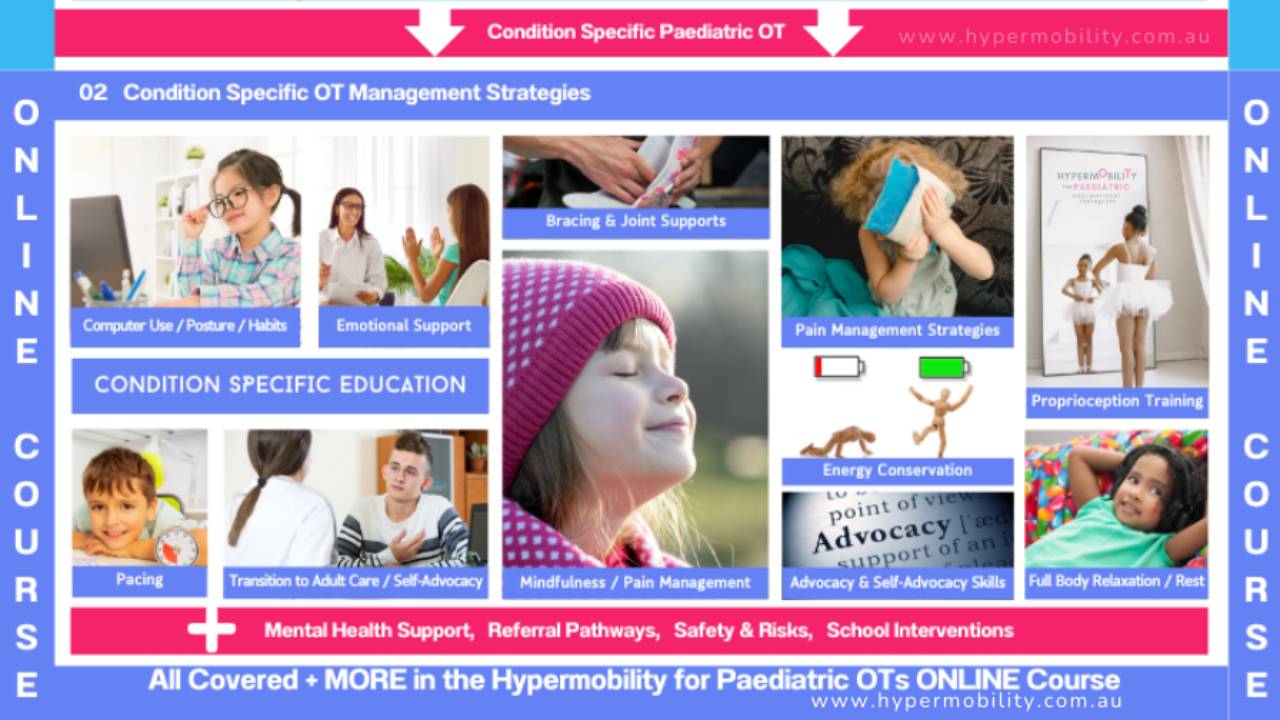
As Paediatric OTs, we focus on functional independence in daily activities such as writing, dressing, eating, and play. We help children manage fine motor difficulties, proprioceptive challenges, and joint instability by recommending ergonomic tools, adaptive equipment, and energy conservation strategies. We also address sensory processing differences, which are common in children with hypermobility, and provide school-based interventions to support learning.
Physiotherapy
Paediatric Physiotherapists are key in improving joint stability, strength, and movement patterns. They focus on low-impact strengthening, proprioception training, and posture correction to reduce pain and prevent injuries. All within the context of play! Physios also educate families on safe movement strategies, helping children participate in physical activities without overloading their joints. They're also great to chat with about sports and physical activity and whether any restrictions are needed to support a child's joints.
Exercise Physiology
Yes, Paediatric EPs exist! An exercise physiologist designs individualised movement programs to help children build muscle endurance, cardiovascular fitness, and motor control. EP aims to improve long-term physical function and participation in activities like sports and recreation, as well as tolerance for physical activity, which can boost confidence and social inclusion.
Psychology
 Living with a chronic condition can impact a child’s mental health, self-esteem, and coping strategies. Many children with hypermobility experience anxiety, fear of movement (kinesiophobia), or social challenges due to their limitations. Psychologists (and appropriately trained Mental Health OTs, Social Workers, Mental Health Nurses) provide emotional support, cognitive-behavioural strategies (CBT), and pain management techniques to help children develop resilience and confidence.
Living with a chronic condition can impact a child’s mental health, self-esteem, and coping strategies. Many children with hypermobility experience anxiety, fear of movement (kinesiophobia), or social challenges due to their limitations. Psychologists (and appropriately trained Mental Health OTs, Social Workers, Mental Health Nurses) provide emotional support, cognitive-behavioural strategies (CBT), and pain management techniques to help children develop resilience and confidence.
Never underestimate the toll pain, fatigue, and disability can have on a child (and their family).
Medical Specialists
Children with hypermobility often require input from rheumatologists, gastroenterologists, paediatricians, and pain specialists (and more) to manage their symptoms. These professionals assist with diagnosis, medication management, and monitoring for associated conditions such as dysautonomia, gastrointestinal issues, and cardiovascular complications.
Dietitian/Nutritionist
Many children with hypermobility have gastrointestinal difficulties, food intolerances, or nutritional deficiencies. Some may also have Mast Cell Activation Syndrome (MCAS) or severe allergies (anaphylaxis). A dietitian helps manage gut health, hydration, and balanced nutrition to support energy levels, muscle function, and overall well-being.
Having the right amount, type and frequency of food and hydration can have a massive impact on a child's ability to engage and participate in their ADLs and meaningful activities.
Team Work
By working together, these professionals ensure a holistic, child-centred approach to managing hypermobility conditions. A coordinated, multidisciplinary plan helps children achieve greater independence, emotional well-being, participation, and quality of life across all aspects of their daily routine. At the end of the day, that's what it's all about!